- Oak Brook:(630) 705-9999
- Chicago:(312) 920-8822
- Email:inquiry@vervecollege.edu
- Make a Payment
- Home
- Programs
- Admission
- Resources
- ATI Entrance Exam Resources
- New E-Digital Library
- Refer a Friend
- School Newsletter
- Events
- Employers
- Job-Network
- Alpha Beta Kappa Candidates
- Verve College Library
- Graduation and Pinning Ceremony Photo Galleries
- Textbook Information
- Career Services
- Tutoring
- School Catalog
- FAQ
- Constitution Day Program
- Alumni
- Verve College Plans
- Financial Aid
- HEERF Reporting
- Satisfactory Academic Progress
- Apply For Financial Aid
- Net Price Calculator
- Return of Title IV Funds (R2T4)
- Financial Aid Office Code of Conduct
- Contact
- FAQs
- Verification Policy
- Vaccination Policy
- Student Right-to-Know Act
- Misrepresentation
- Information Security Program
- Academic Award Year
- Availability of Employee
- Cost of Attendance
- Health & Safety Exemption Requirement
- Students Rights and Responsibilities
- Leave of Absence
- Pell Formula
- Military Students
- Grants/ Scholarship Policy
- Contact Us
- Testimonials
- Blog
Is a Nursing Career Right For You?
Take The Free Quiz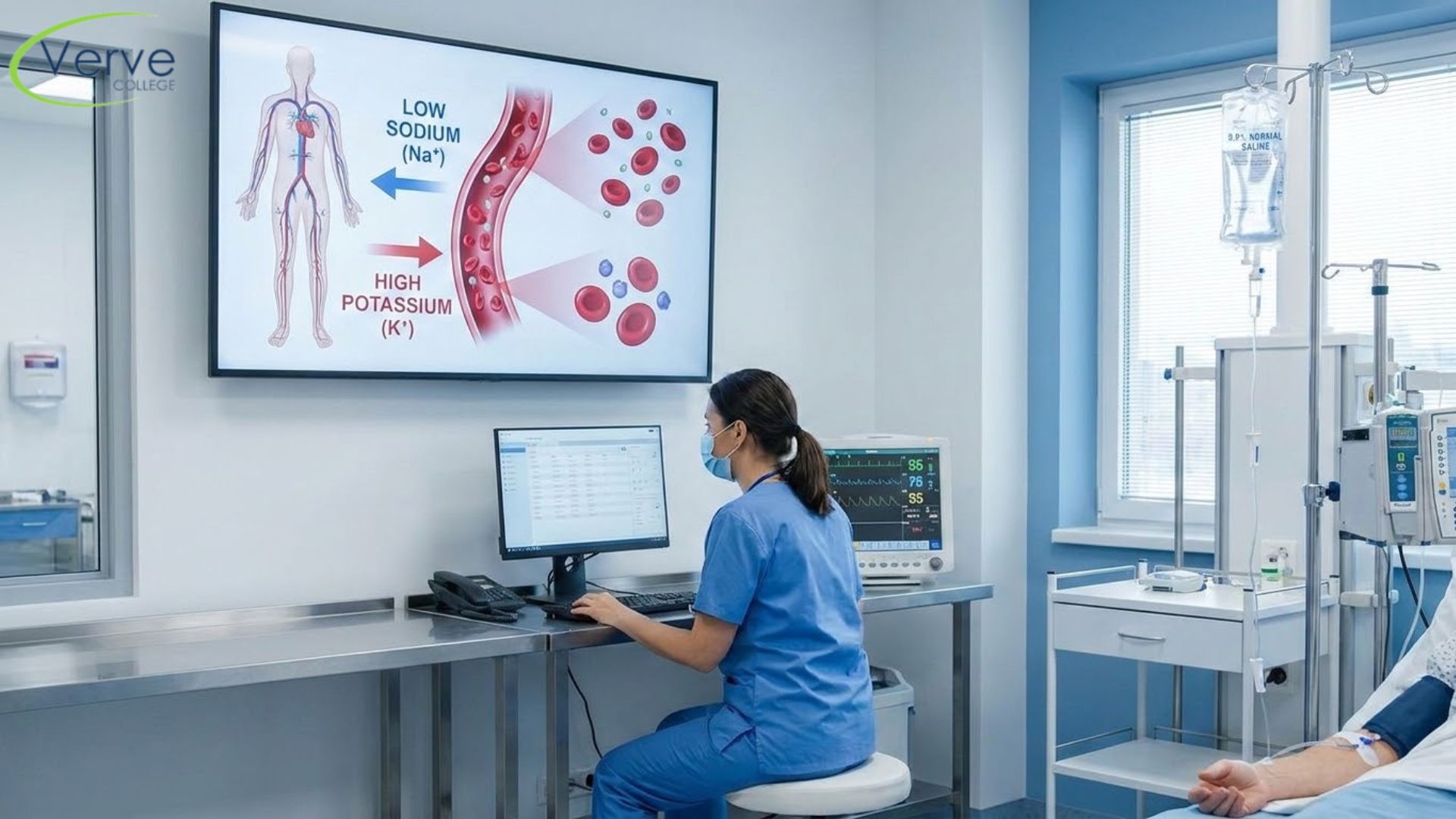
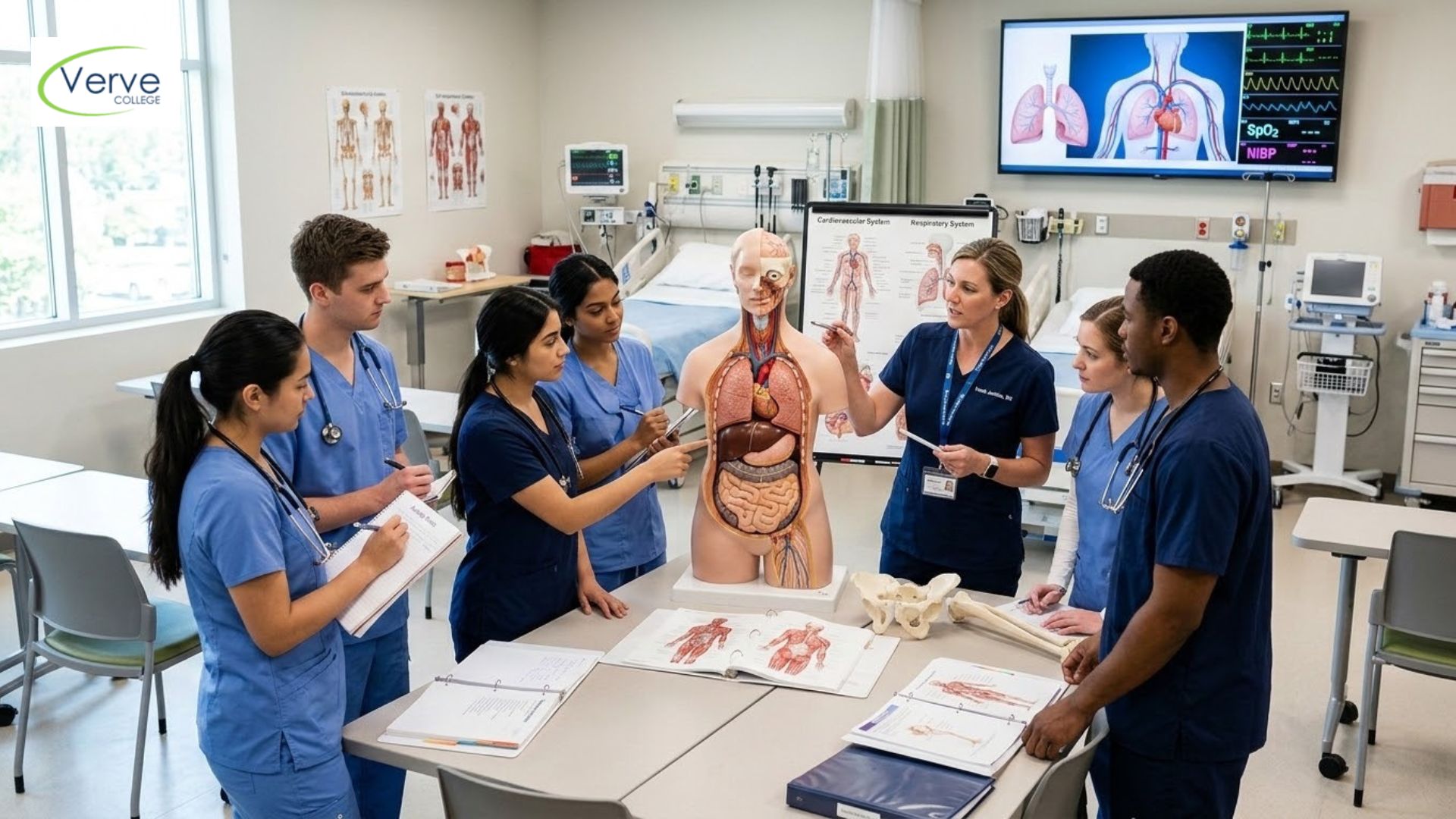
Fluid and Electrolyte Imbalances: What Every Nurse Needs to Know
Fluid and Electrolyte Imbalances: What Every Nurse Needs to Know
Your patient’s sodium level just came back dangerously low. Do you know what to watch for next? Fluid and electrolyte imbalance nursing is one of the most commonly tested areas on the NCLEX-PN, and for good reason. These imbalances show up in almost every clinical setting, from long-term care to emergency rooms. This guide breaks down the essentials so you can walk into your first shift with real confidence.
Key Takeaways
- Fluid and electrolyte imbalances are a core nursing topic and appear frequently on NCLEX-PN exams
- The most clinically important electrolytes to know are sodium, potassium, calcium, and magnesium
- Early recognition of symptoms is more important than memorizing lab values alone
- Hyponatremia and hyperkalemia are two of the most dangerous and frequently seen imbalances
- Nurses play a central role in monitoring, reporting, and responding to these changes
- Students enrolled in LPN programs learn how to connect classroom theory to real patient scenarios
Why Fluid and Electrolyte Balance Matters in Nursing
The human body runs on balance. Every cell, organ, and system depends on the right amount of fluid and the right concentration of electrolytes to function properly. When that balance shifts, even slightly, patients can deteriorate quickly.
Electrolytes are minerals in your blood and body fluids that carry an electrical charge. Sodium, potassium, calcium, chloride, and magnesium are the main ones nurses monitor. Each plays a different role in keeping the heart beating, muscles contracting, and nerves firing correctly.
As a nurse, you will not just be reading lab results. You will be the one at the bedside noticing when something feels off before the numbers confirm it. That is why understanding these imbalances goes beyond memorization.
The Most Common Fluid Imbalances
Dehydration
Dehydration happens when the body loses more fluid than it takes in. It can result from vomiting, diarrhea, fever, sweating, or simply not drinking enough.
Signs include dry mouth, decreased urine output, concentrated (dark yellow) urine, low blood pressure, and increased heart rate. In older adults, confusion is often an early warning sign that gets missed.
Fluid Overload
Fluid overload, also called hypervolemia, is the opposite. Too much fluid builds up in the body. This is common in patients with heart failure or kidney disease.
Look for swelling in the legs and ankles, shortness of breath, crackles in the lungs when you listen with a stethoscope, and rapid weight gain. Catching this early prevents serious complications.
Key Electrolyte Imbalances Every LPN Should Know
Hyponatremia (Low Sodium)
Hyponatremia means the sodium level in the blood is too low, typically below 135 mEq/L. Sodium controls how much water stays in and around cells, so when it drops, cells can swell.
Symptoms include nausea, headache, confusion, fatigue, and in severe cases, seizures or coma. Hyponatremia nursing assessment starts with watching for neurological changes in patients who are on diuretics, have kidney issues, or are drinking excessive amounts of water.
Hypernatremia (High Sodium)
Hypernatremia is when sodium rises above 145 mEq/L, usually because of dehydration or inadequate fluid intake. The brain is especially vulnerable.
Patients may appear restless, confused, or extremely thirsty. Skin becomes dry and flushed. Elderly patients and those who cannot communicate thirst clearly are at higher risk.
Hypokalemia (Low Potassium)
Potassium is essential for heart and muscle function. When it drops below 3.5 mEq/L, muscle weakness, cramping, and abnormal heart rhythms can follow.
Watch for fatigue, constipation, irregular pulse, and muscle cramps. Patients taking diuretics are at elevated risk and need regular monitoring.
Hyperkalemia (High Potassium)
Hyperkalemia symptoms appear when potassium rises above 5.0 mEq/L. This is one of the most dangerous electrolyte disorders because it can cause life-threatening heart arrhythmias.
Key signs include muscle weakness, numbness, slow heart rate, and in severe cases, cardiac arrest. Patients with kidney failure are particularly vulnerable because the kidneys regulate potassium excretion.
Hypocalcemia and Hypercalcemia
Calcium affects muscle contraction, nerve transmission, and bone health. Low calcium (hypocalcemia) can cause muscle spasms, numbness around the mouth, and a positive Trousseau sign (hand spasm when a blood pressure cuff is inflated).
High calcium (hypercalcemia) often presents more subtly with fatigue, constipation, nausea, and bone pain. Patients with certain cancers or overactive parathyroid glands are most at risk.
Magnesium Imbalances
Magnesium is less talked about but just as important. Low magnesium can cause tremors, confusion, and seizures. High magnesium leads to muscle weakness, low blood pressure, and slowed breathing.
These imbalances often occur alongside other electrolyte disorders, so always think about the whole picture.
How Nurses Assess and Respond
Recognizing symptoms is step one. Step two is knowing how to respond.
As an LPN, your role includes monitoring lab values, reporting changes to the supervising nurse or physician, adjusting fluid intake based on care plan instructions, and documenting everything accurately.
You are not expected to diagnose these conditions. You are expected to notice the warning signs, communicate clearly, and follow the care plan precisely. That is what makes a skilled practical nurse genuinely valuable.
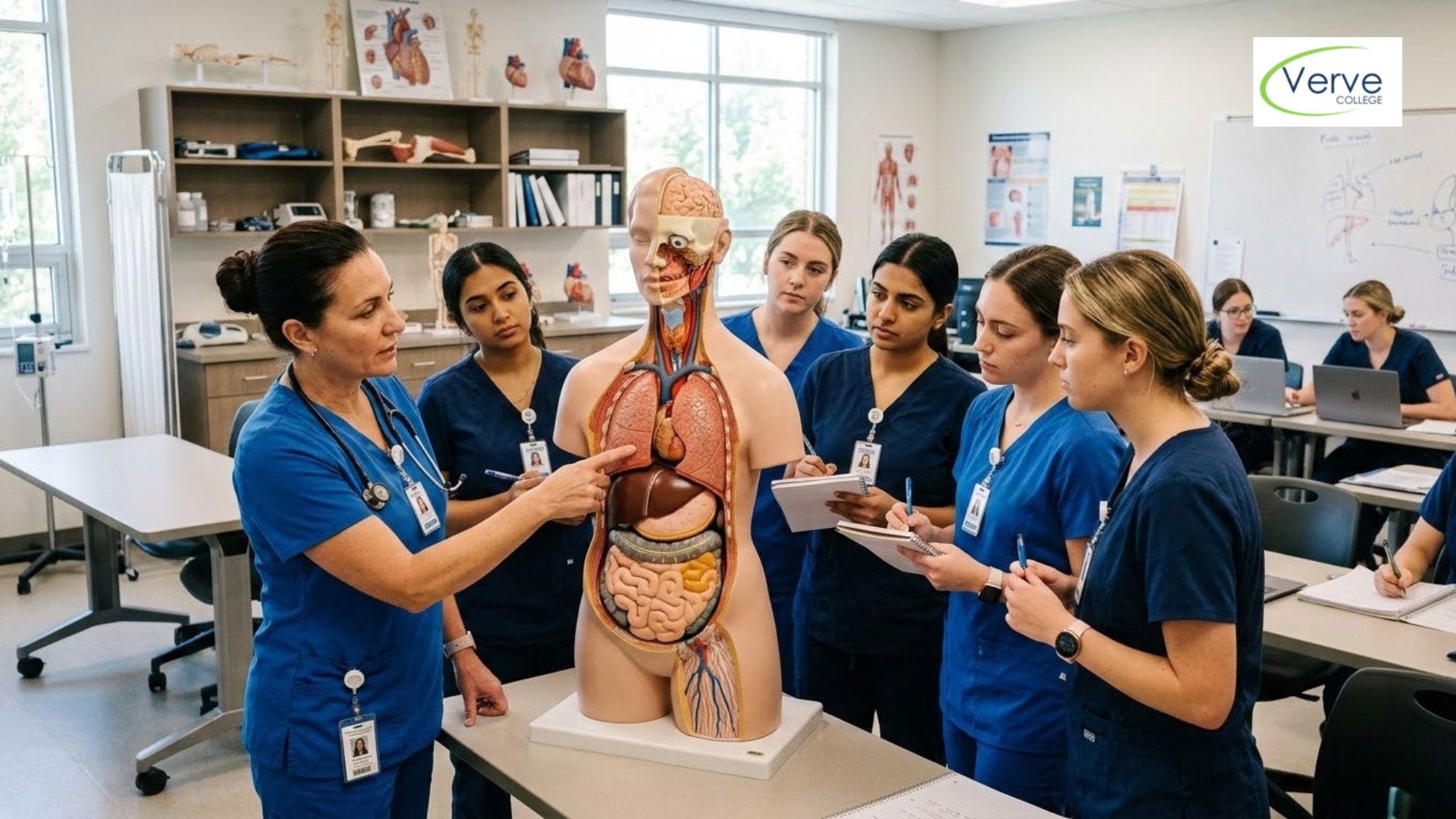
Strong assessment skills begin with understanding how the body works from the inside. Students who build a solid foundation through anatomy and physiology classes tend to connect these dots much faster in clinical settings.
Common Mistakes Students Make With This Topic
One of the most common errors is focusing only on lab values and ignoring the patient in front of you. Lab numbers confirm what is happening, but symptoms often show up first.
Another mistake is treating each electrolyte in isolation. Sodium, potassium, and fluid levels are closely connected. A drop in one often triggers a shift in another.
Finally, do not underestimate how much medication affects electrolyte balance. Diuretics, laxatives, corticosteroids, and certain antibiotics can all cause significant shifts. Knowing a patient’s medication list is part of the assessment.
Building the Skills to Handle These Situations
Fluid and electrolyte imbalances are not just a test topic. They are a real, daily part of nursing practice. The faster you can recognize and respond to them, the better your patients will do.
A strong clinical education gives you the tools to connect what you learn in the classroom to what you see at the bedside. If you are ready to develop those skills in a structured, hands-on environment, exploring accredited LPN programs can help you find the right path forward.
Conclusion
Fluid and electrolyte imbalance nursing is a topic every aspiring LPN needs to take seriously. From hyponatremia to hyperkalemia, these conditions are common, clinically significant, and entirely manageable when you know what to look for. The goal is not to memorize every value but to develop the habit of observing, connecting, and acting. Master that skill early and you will carry it through your entire nursing career.
Get Your Nursing Career Training Readiness Score Now!
FAQs
- What are the most important electrolytes for nurses to monitor?
Sodium, potassium, calcium, and magnesium are the four electrolytes most frequently monitored in clinical nursing. Each plays a different role in heart, muscle, and nerve function, and imbalances in any of them can cause serious symptoms quickly.
- How do I know if a patient’s confusion is caused by an electrolyte imbalance?
Confusion can have many causes, but sudden or unexplained changes in mental status in a patient with a history of kidney disease, dehydration, or certain medications should always prompt a check of their electrolyte levels. Report the change to your supervising nurse right away and document what you observed and when.
- Do LPN programs cover fluid and electrolyte imbalances in depth?
Yes. Practical nursing programs include pharmacology, medical-surgical nursing, and anatomy content that all touch on electrolyte balance. The level of depth varies by program, but accredited programs ensure students understand how to recognize and respond to common imbalances before entering clinical practice.
 Sign up
Sign up Login
Login